Accurate & Timely Claims Submission
- Promdix provides reliable Claims Submission services designed to ensure that healthcare providers receive timely reimbursement for their services. Accurate claim submission is a critical part of the revenue cycle, as errors in coding, patient information, or documentation can result in denials, delays, or revenue loss.
- Our experienced billing specialists handle all aspects of claim preparation and submission, ensuring that every claim is complete, compliant, and submitted according to payer guidelines.

Streamlined Claims Processing for Maximum Efficiency
Efficient claims submission improves cash flow and minimizes administrative burden. Promdix uses structured workflows and quality checks to prepare claims accurately and submit them electronically or via paper, depending on payer requirements.
By ensuring proper coding, documentation, and eligibility verification, we reduce rejections, speed up reimbursements, and improve first-pass claim acceptance rates.
- Accurate coding and charge entry verification
- Timely electronic and paper claim submission
- Compliance with payer-specific guidelines
- Reduced claim denials and rejections
- Improved first-pass claim approval rate
- Transparent tracking and reporting of claims
Our Claims Submission Services
Eligibility & Insurance Verification
Confirm patient coverage and payer requirements prior to claim submission.
Charge & Documentation Review
Ensure all codes, modifiers, and supporting documents are accurate and complete.
Electronic Claim Submission
Efficient submission of claims via clearinghouses or direct payer portals.
Paper Claim Preparation
Accurate preparation of manual claims when electronic submission is not available.
Denial Prevention
Identification of potential errors before submission to minimize claim rejections.
Claims Tracking & Follow-Up
Monitoring of claim status and proactive follow-up to expedite payments.
Why Choose Promdix for Claims Submission?
Promdix combines billing expertise with advanced workflow processes to ensure claims are submitted accurately, efficiently, and on time. Our team acts as an extension of your practice, reducing administrative burden while protecting revenue.
With Promdix handling claims submission, healthcare providers can focus on patient care while enjoying improved cash flow and minimized claim rejections.
- Certified billing specialists
- High first-pass claim acceptance rate
- Reduced administrative workload
- Compliance with HIPAA and payer regulations
- Seamless integration with EHR and PM systems
- Transparent reporting and analytics
Frequently Asked Questions
What is claims submission in medical billing?
Claims submission is the process of sending patient service claims to insurance payers for reimbursement.
Why is accurate claims submission important?
Errors in claims can lead to denials, payment delays, and revenue loss.
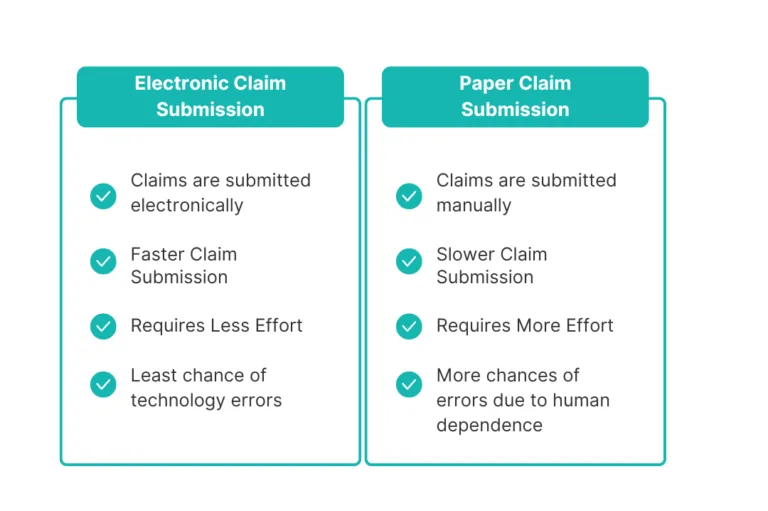
Do you handle both electronic and paper claims?
Yes, we submit claims electronically or via paper, depending on payer requirements.
How do you prevent claim denials?
We verify eligibility, review charges and documentation, and follow payer-specific guidelines before submission.
Can you track claim status after submission?
Absolutely. We provide regular tracking and follow-up to ensure timely reimbursement.
Is patient data secure during the submission process?
Yes, all claims submission processes are HIPAA-compliant and securely handled.
Ready to Simplify Your Medical Billing?