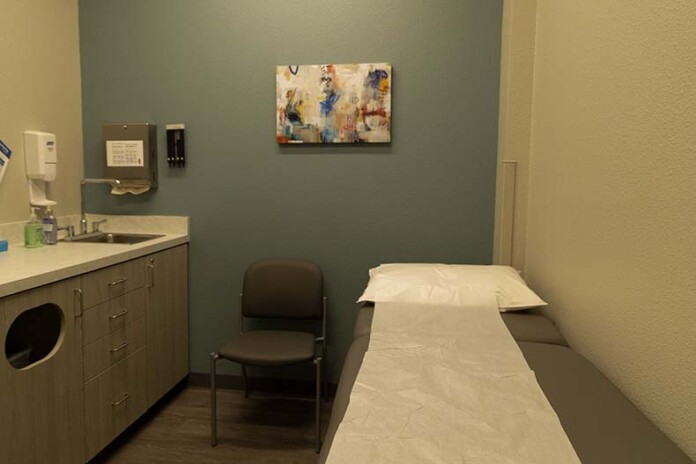
Professional Urgent Care Medical Billing Services Across the United States
- Urgent care centers operate in a fast-paced healthcare environment where efficiency, accuracy, and speed directly affect revenue. Unlike traditional practices, urgent care facilities manage walk-in patients, same-day treatments, occupational health visits, minor procedures, and varying insurance plans—all of which require precise billing workflows. At Promdix, we provide specialized Urgent Care medical billing services in the United States designed to streamline revenue cycle operations, reduce claim denials, and optimize reimbursements.
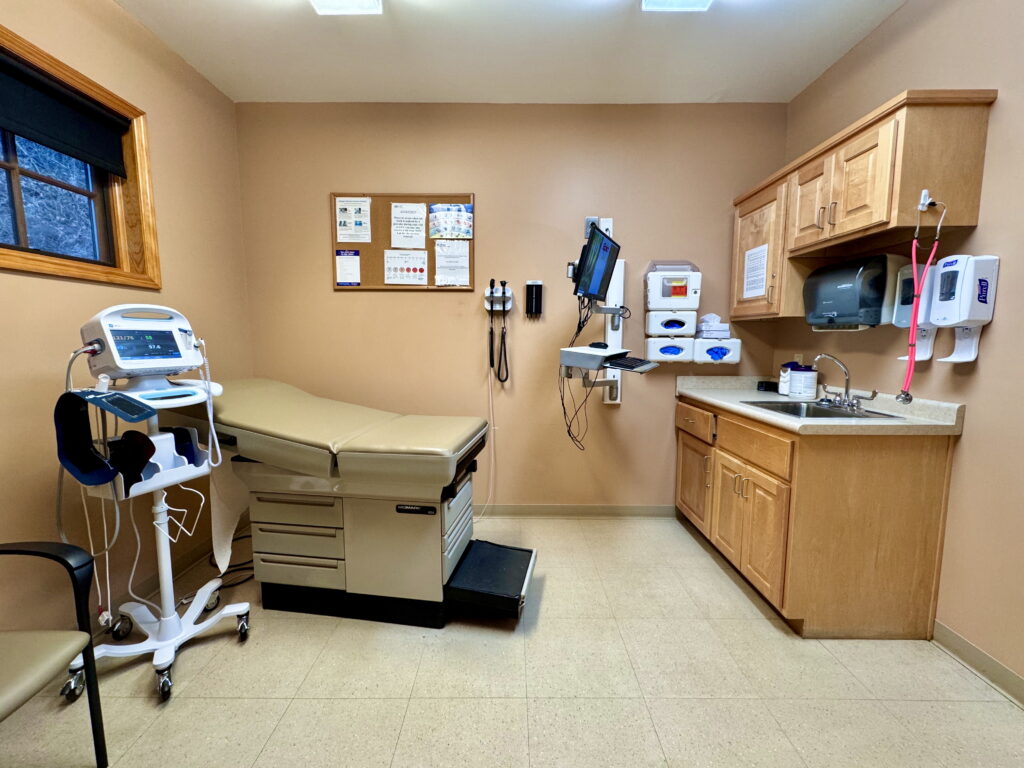
Optimized Revenue Cycle Management for Urgent Care Centers
Promdix offers comprehensive revenue cycle management solutions tailored specifically for urgent care clinics across the U.S. healthcare system. We manage every stage of the billing lifecycle, including insurance eligibility verification, prior authorizations when required, accurate charge capture, coding validation, electronic claim submission, and payment posting. Our structured process minimizes front-end errors and improves first-pass claim acceptance rates.
In addition to claim submission, we provide proactive denial management and accounts receivable follow-up to recover unpaid or underpaid claims. Our billing specialists monitor payer trends, reimbursement patterns, and aging reports to ensure urgent care providers experience improved collections and reduced administrative burden.
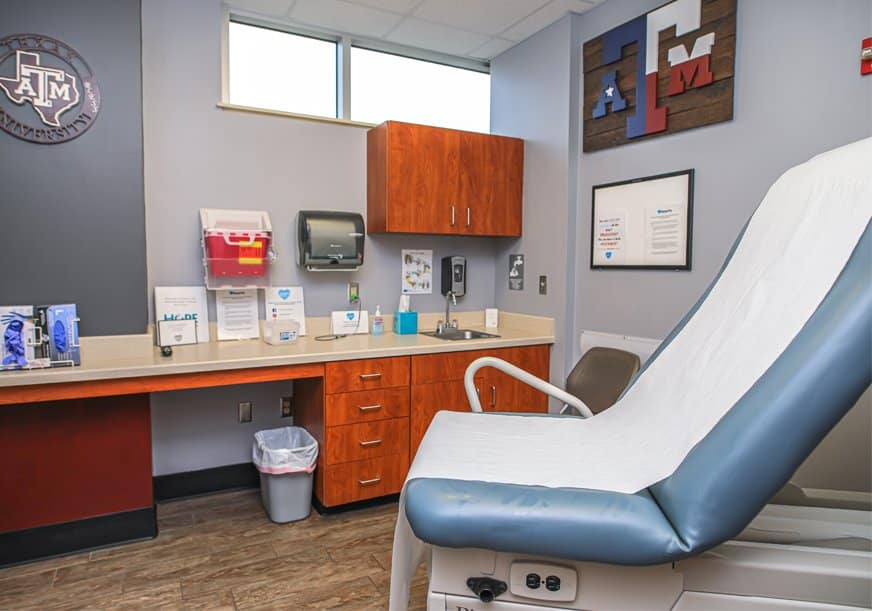
Dedicated Billing Expertise for High-Volume Walk-In Clinics
Urgent care billing demands rapid claim processing, accurate documentation review, and strict compliance with evolving payer regulations.
Fast Turnaround
We accelerate claim processing cycles to reduce reimbursement delays and maintain steady revenue flow for urgent care clinics nationwide.
Coding Precision
Our certified coders apply accurate E/M levels, procedure codes, and modifiers to reduce denials and improve claim acceptance rates.
Denial Resolution
We investigate denied claims, correct documentation discrepancies, and submit timely appeals to recover maximum eligible reimbursements.
Insurance Verification
We perform detailed eligibility checks before services to prevent coverage issues and minimize claim rejections.
Compliance Security
Our billing processes follow HIPAA regulations and CMS guidelines to protect patient data and ensure legal compliance.
Financial Reporting
We provide transparent revenue reports and performance analytics to support strategic decision-making and operational growth.
Secure, Compliant, and Performance-Driven Billing Solutions
Maintaining regulatory compliance is essential in urgent care billing due to diverse payer requirements and federal healthcare laws. Promdix follows strict HIPAA protocols and CMS standards to safeguard patient information and ensure billing accuracy.
Our internal quality assurance reviews continuously evaluate coding integrity, reimbursement trends, and documentation standards. This proactive oversight strengthens trust, improves financial predictability, and positions urgent care providers for sustainable long-term growth across competitive U.S. healthcare markets.